In the wake of the COVID-19 pandemic, medical complexities have emerged, and the case of a young patient with avascular necrosis (AVN) in both hips following COVID-19
infection stands as a testament to the challenges faced in post-pandemic orthopedic care.
This case study delves into the journey of a patient who underwent a series of surgeries to address complications arising from a previously performed cemented total hip replacement.
Case Background:
The patient, a young individual, had undergone a cemented total hip replacement in another facility a month prior to presenting with complaints of persistent pain and
discomfort over a seven-month period.
The situation escalated dramatically, with the patient experiencing increased pain, ultimately leading to the inability to walk on the left lower limb.
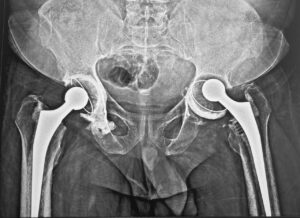
Diagnostic X-rays revealed cup loosening in the left hip joint, necessitating immediate intervention.
Treatment Course:
Upon careful evaluation, a two-stage surgical approach was deemed necessary.
The initial stage involved the removal of the primary implant, excision of necrotic tissue, and the insertion of an antibiotic cement spacer to combat infection.
Subsequently, after a period of six weeks, the patient, upon showing signs of improvement and stabilization, was readmitted for further intervention.
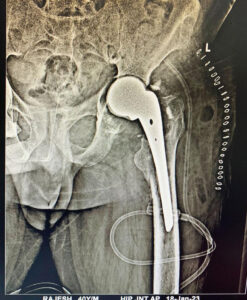
The second stage of surgery involved the removal of the antibiotic cement spacer and the implementation of a mega prosthesis with a Vagnar stem made of porous titanium.
This advanced prosthetic approach aimed to provide structural stability and facilitate the patient’s mobility and function.
Challenges and Recovery:
The complexity of this case was multifaceted, including the intricacies of post-COVID complications, avascular necrosis, implant loosening, and the necessity for a staged
surgical approach.
The patient’s recovery journey was characterized by resilience, determination, and collaborative efforts among the medical team.
Outcome:
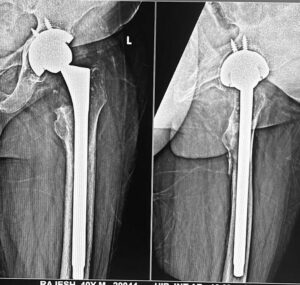
Post the second stage of surgery, the patient demonstrated promising signs of recovery.
Follow-up assessments indicated reduced pain, improved joint stability, and an enhanced ability to walk and perform daily activities.
The use of advanced prosthetic technology, coupled with meticulous surgical intervention and a comprehensive rehabilitation program, contributed significantly to the patient’s positive outcomes.
Conclusion:
The case highlights the intricate challenges in managing post-COVID orthopedic complications, emphasizing the importance of a multidisciplinary approach, precision in
surgical techniques, and the utilization of advanced prosthetic options.
This successful case serves as a beacon of hope, showcasing the potential for recovery and restoration of functionality in complex orthopedic scenarios even amidst challenging circumstances.
The patient’s journey underscores the significance of tailored treatment plans, ongoing monitoring, and the unwavering resilience of both patients and medical professionals in the face of adversity.